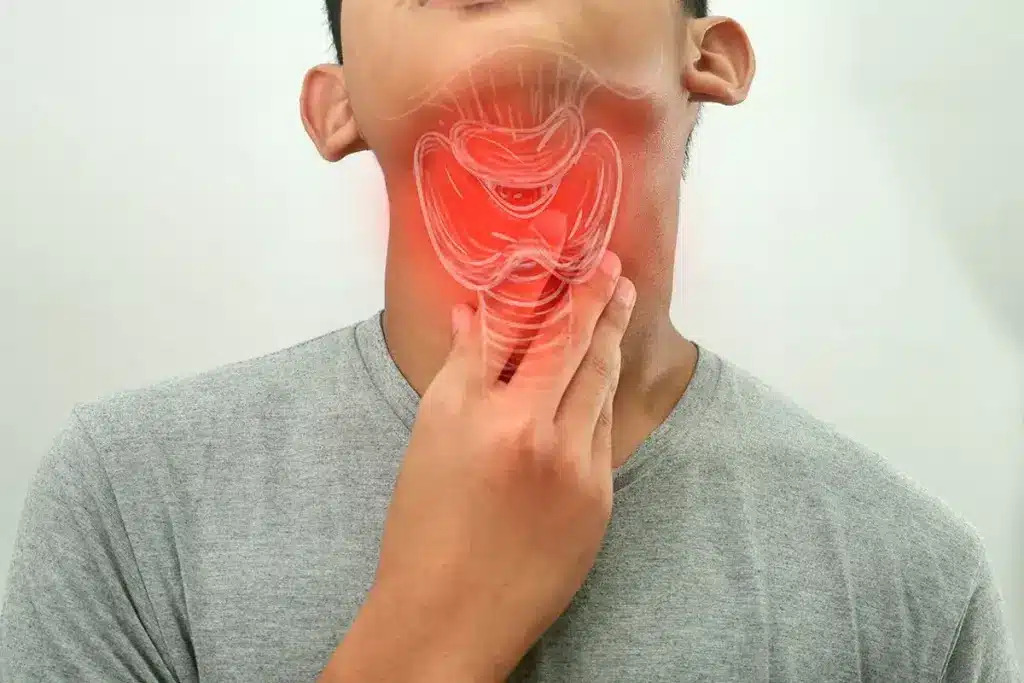
The first time I had tonsillitis strep throat simultaneously, I genuinely thought I was being dramatic. I’d had sore throats before plenitude of them and this felt like perhaps a bad one, perhaps a really bad one, and I kept telling myself to just drink further water and stop catastrophizing. That particular brand of denial lasted about eighteen hours before I could not turn my head without quailing and my fever had climbed grandly enough that my hands were shaking when I eventually picked up the phone to call my croaker.
Tonsillitis strep throat is a bacterial infection that causes a severe sore throat, blown tonsils, difficulty swallowing, and fever. Prompt medical attention is essential, as undressed infections can lead to serious complications like rheumatic fever or order issues. Early opinion and a full course of antibiotics help cases recover briskly while reducing the threat of spreading the infection. Managing tonsillitis strep throat effectively ensures hastily relief and safer recovery.
Stay tuned with us as we explore tonsillitis strep throat, participating in essential tips and treatment advice for briskly, safer recovery.
What Tonsillitis Strep Throat Actually Is and Why It Hits So Hard:
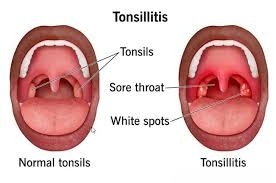
This condition sounds like one thing but it’s actually the imbrication of two affiliated but distinct conditions that constantly do together and produce a combined donation more severe than either alone. Tonsillitis is inflammation of the tonsils of those two round- shaped lymph towel pads sitting at the reverse of your throat which can be touched off by contagions, bacteria, or both contemporaneously. Strep throat is a bacterial infection caused specifically by Group A Streptococcus populating the throat filling and girding towel. When strep is the bacteria causing the tonsil inflammation, you get tonsillitis strep throat and that combination tends to hit harder, last longer without treatment, and carry an advanced complication threat than viral tonsillitis alone.
The tonsils are actually part of the vulnerable system designed to catch and fight pathogens entering through the mouth and nose, which explains why they are deposited exactly where they are. The cruel irony is that the very tissue meant to protect you from bacterial infection becomes the primary site of that infection when Group A Streptococcus overwhelms its defenses. Tonsils swell dramatically, sometimes nearly touching each other what doctors call “kissing tonsils” and white or yellow pus-filled patches develop on their surface as the immune battle intensifies. Understanding this biology helps explain why this particular infection feels so acutely awful in ways ordinary sore throats simply don’t.
How This Infection Spreads and Who Gets It Most:
The condition does not materialize from nowhere it spreads through direct contact with an infected person’s respiratory driblets, meaning coughing, sneezing, participating implements, participating drinks, or close discussion with someone laboriously slipping bacteria can be enough for transmission. The incubation period generally runs two to five days, creating this maddening situation where you can pinpoint roughly when exposure happened but infrequently exactly who gave it to you. Tonsillitis strep throat moves efficiently through households, classrooms, offices, and anywhere people spend extended time in close proximity.
Children between five and fifteen are statistically the most affected age group; their immune systems are still developing, they’re in daily close contact with dozens of other children, and hygiene habits at that age are generously described as inconsistent. Adults get it with meaningful frequency too, particularly parents of school-age children who function as continuous exposure vectors bringing bacteria home regularly. People working in healthcare, education, or high-contact professions face elevated risk compared to those in low-density work environments. This infection doesn’t discriminate particularly; it just finds dense, close-contact environments significantly easier to move through than isolated ones.
Recognizing Tonsillitis Strep Throat Symptoms Before They Reach Full Peak:
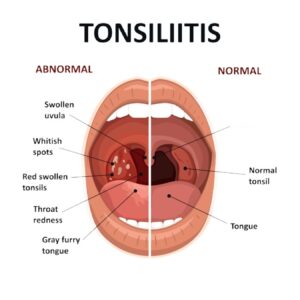
The recognition piece is where most people including past me lose the most ground. Tonsillitis strep throat caught at the first sign of symptoms and treated within 24 hours feels dramatically different from the same infection brewing for three days before anyone reaches for a phone. Early signs are subtle enough to rationalize away, which is exactly what most people do, and exactly what costs them days of unnecessary suffering they didn’t need to experience.
Opening Symptoms That Arrive Fast and Without Warning:
This condition almost never builds gradually the way a viral cold does. Onset is characteristically sudden, fine in the morning, noticeably off by afternoon, genuinely unwell by evening. Throat pain comes sharp and specific rather than the verbose scratchiness of a viral sore throat. Fever follows snappily, frequently climbing to 101 or 102 degrees within hours. Swallowing becomes decreasingly delicate as tonsils begin swelling, and indeed drinking water thresholds take conscious trouble and decision- timber. Catching tonsillitis strep throat at this early stage produces the fastest, cleanest recovery when treatment starts incontinently.
The Middle Phase When Everything Feels Worse:
By day two or three without treatment, the full inflammatory picture is usually established. Tonsils are visibly swollen and may show white or yellowish patches of exudate on their surface. Lymph nodes in the neck are tender and palpable even to the patient’s own touch. Fever fluctuates rather than staying consistently high. Headache and body aches join the throat symptoms, and fatigue becomes the kind that makes getting off the couch feel genuinely unreasonable. The condition responds well to antibiotics at this stage but recovery takes longer than it would have with earlier intervention.
Signs That Tell You Things Are Becoming Dangerous:
Not every case moves cleanly toward resolution even with treatment. A subset develops complications peritonsillar abscess being most common requiring intervention beyond standard oral antibiotics. If throat pain becomes dramatically worse rather than gradually better after 48 hours on medication, if pain is significantly more severe on one side, if there’s visible tissue bulging to one side, or if jaw stiffness develops — these signs mean tonsillitis strep throat has moved past straightforward territory and needs same-day medical evaluation without delay.
Home Remedies That Genuinely Help Recovery:
Home remedies Live in two orders in my experience: effects that actually do commodity measurable and effects that feel nice but are substantially comfortable. Both have a place, but knowing which is which helps you invest limited sick- day energy in the bones that actually move the recovery needle rather than the bones that just feel probative.
Salt Water Gargling Done Right Makes a Real Difference:
Half a tablespoon of swab dissolved in eight ounces of warm water, gargled for thirty seconds and repeated every two to three hours. This sounds simple but most people do it formally, decide it’s not working, and quit. The medium is real swab water temporarily reduces facial bacterial cargo, decreases mucosal lump, and loosens debris from inflamed tonsil towel that contributes directly to pain and swallowing difficulty. It does not treat the underpinning infection, but it makes the face terrain meaningfully less sociable to bacteria and noticeably more comfortable when done with genuine thickness throughout the day.
Raw Honey and Warm Liquid Address More Than Just Comfort:
Raw honey, specifically Manuka or another high-quality unprocessed variety contains antimicrobial compounds including methylglyoxal with legitimate research support for activity against bacterial pathogens. Dissolved in warm chamomile or ginger tea, it coats inflamed tonsil tissue, reduces the dry scratching sensation that makes this infection so sleep-disruptive, and provides temporary protective coating that reduces friction from swallowing. I went through an embarrassing amount of Manuka honey during my second and third bouts with tonsillitis strep throat. It didn’t cure anything except antibiotics does that but it made the experience significantly less miserable hour by hour throughout recovery.
Cold Foods Offer Targeted Relief Worth Knowing About:
This surprised me because everything I’d read suggested warm liquids exclusively. But cold foods, ice chips, cold water, ice cream, firmed fruit, popsicles reduce original inflammation in blown tonsil towels through vasoconstriction in a way warm liquids do n’t. Cold provides temporary deadening making eating and drinking easier, which matters because staying doused and maintaining some sweet input is authentically important for vulnerable function and recovery speed. Alternating warm honey tea with ice chips addresses both the soothing benefit of warmth and the anti-inflammatory benefit of cold simultaneously.
Why Antibiotics Are Non-Negotiable for This Condition:
This is what I feel most strongly about because I’ve watched well-intentioned people try managing this purely with natural remedies and suffer significantly more and longer than necessary. Tonsillitis strep throat caused by Group A Streptococcus is a bacterial infection, and bacterial infections respond to antibiotics in ways they simply don’t respond to anything else. The research is not ambiguous. Antibiotics dock symptom duration, reduce pain briskly, cut the contagious period from potentially weeks to 24 hours, and most importantly exclude conditions that allow rheumatic fever and other serious complications to develop.
Penicillin remains first- line treatment after seven decades of use, remarkable given how snappily bacteria generally evolve resistance. Group A Streptococcus has shown nearly no clinically meaningful penicillin resistance, meaning when your croaker prescribes it for verified tonsillitis strep throat, the outgrowth is as close to certain as drug gets. Amoxicillin is often preferred for practically better taste for children and once-daily dosing options that improve completion rates. The ten-day course feels long at day four when you feel largely human again. Finish it anyway. Cases appearing to resolve but cut short on antibiotics relapse with frustrating frequency, and the second round is often harder than the first.
Five Habits Making Recovery Slower Than Necessary:
Most people focus on what to do. These are the things to stop doing habits that actively slow recovery, increase complication risk, and extend suffering beyond what sensible management would cause.
- Stopping antibiotics when you feel better rather than when they’re finished surviving bacteria at day four are not cleared bacteria. They regroup, re-establish, and produce relapses that are frequently more stubborn than the original and sometimes require a longer or different antibiotic course to finally clear. This single mistake explains a significant portion of recurrent tonsillitis strep throat cases that doctors see repeatedly throughout the year.
- Returning to normal exertion before the 24- hour post-antibiotic window closes cases remain contagious until at least 24 hours after starting antibiotics and fever-free for 24 hours. Going back to work or academy before this window closes spreads bacteria to people who had no say-so in their exposure, while physical demands contemporaneously decelerate the vulnerable response at exactly the moment it needs doing its utmost ferocious work.
- Using commercial antibacterial mouthwash thinking it helps this seems logical but backfires in practice. Antibacterial mouthwash disrupts the oral microbiome indiscriminately, eliminating beneficial bacteria that help maintain throat environment balance. The disruption can prolong recovery rather than accelerating it, while salt water achieves surface-clearing benefits without the microbiome disruption commercial products cause.
- Under- hydrating because swallowing is painful, accessible but authentically ineffective. Dehumidification during infection thickens concealment, worsens fever, slows lymphatic drainage, and makes the throat drier and further painful — a tone- buttressing cycle making everything worse. Staying ahead of fluid input indeed when every swallow is uncomfortable is one of the most poignant effects any case can do to meaningfully support recovery speed.
- Not replacing your toothbrush on day one of antibiotic treatment Group A Streptococcus survives on toothbrush bristles and reintroduces bacteria to a healing throat twice daily during the most critical recovery phase. It’s a two-dollar fix most people never think about, and it’s one of the more reliable explanations for people getting sick again within weeks of what felt like successful treatment completion.
Five Tonsillitis Strep Throat Warning Signs Needing Emergency Attention:
These aren’t “be cautious” signals; these are call-the-doctor-today or go-to-the-ER signals. Any of these signs appearing means tonsillitis strep throat has moved past territory where home management and oral antibiotics are sufficient responses.
- Throat pain intensifying rather than improving after 48 to 72 hours on antibiotics improvement should be happening by this point, not regression. Worsening pain after starting treatment suggests either the antibiotic isn’t matched to your specific strain, or peritonsillar abscess is forming a complication requiring drainage that cannot be resolved by continuing the current oral course alone.
- Dramatically worse pain on one side with visible tissue bulging asymmetric swelling with unilateral pain escalation is classic peritonsillar abscess presentation. The abscess is a pus collection forming between the tonsil and surrounding pharyngeal tissue, significantly more painful than the original infection patients often describe as the worst throat pain they’ve ever experienced by a meaningful margin.
- Jaw stiffness or difficulty opening the mouth fully trismus in this context is an urgent signal indicating abscess formation or deeper tissue involvement. Same-day evaluation is appropriate — waiting overnight to see if it improves is not a reasonable approach to this specific symptom combination under any circumstances whatsoever.
- High fever returning after originally perfecting on antibiotics a biphasic fever pattern suggests either shy antibiotic response, secondary infection development, or arising complications. This warrants a same- day call rather than covering at home for another 24 hours hoping effects resolve in the right direction on their own.
- Difficulty breathing or sensation of throat closing severely swollen tonsils can narrow the airway in extreme cases, creating genuine breathing difficulty representing a medical emergency. Any breathing compromise associated with this infection warrants emergency services rather than urgent care or a scheduled appointment the following morning.
Recurrent Tonsillitis Strep Throat Cases and When Surgery Becomes the Right Answer:
This section applied most directly to my situation after my third recurrence. When do you stop treating each episode individually and start asking whether the tonsils themselves have become a structural liability rather than an asset? Recurrent tonsillitis strep throat is generally defined as five or more confirmed strep infections per year for two consecutive years, or seven or more in a single year. At that frequency, tonsils have generally come chronically infected towel harboring bacteria between acute occurrences, a force for repeated infection rather than the vulnerable defense they were firstly designed to give.
Tonsillectomy is not as generally performed as in former decades when it was nearly reflexively recommended for any child with repeated throat infections. Current guidelines are more picky, reserving it for cases authentically meeting rush thresholds or where quality of life impact, complications, or airway enterprises make it easily applicable. For patients meeting those criteria, surgery reduces tonsillitis strep throat incidence dramatically, not completely eliminating strep risk since remaining throat tissue can still be infected, but removing chronically affected tissue that has become the primary infection site. My ENT put it plainly: in patients with chronic recurrence, the tonsils have stopped being part of the solution and become part of the problem entirely.
What Happens When Tonsillitis Strep Throat Goes Untreated Too Long:
I want to be specific here rather than vague, because vague scary health information isn’t actually useful to anyone trying to make real decisions. Undertreated or untreated tonsillitis strep throat doesn’t just mean a longer, more miserable version of normal recovery it means specific, documented complications significantly more serious than the original infection.
Rheumatic fever develops in a subset of undressed cases an autoimmune seditious response touched off by the strep bacteria that can beget carditis, common inflammation, and in serious cases endless heart stopcock damage that does not reverse with late treatment.
Post-streptococcal glomerulonephritis is an order complication involving vulnerable complex deposits causing blood in urine and dropped order function. Peritonsillar abscess requires drainage rather than antibiotics alone. Retropharyngeal abscess infection spreading to towel behind the throat is rarer but more serious, occasionally taking surgical drainage and dragged IV antibiotic treatment. A full antibiotic course for tonsillitis strep throat avoids basically all of these complications entirely. The ten- day course is not pharmaceutical assiduity preference — it’s the duration that reliably prevents these issues across the broader patient population.
Conclusion
Tonsillitis strep throat is authentically one of the further treatable serious infections that exists — caught beforehand, treated duly, managed with smart probative care, it resolves fairly and leaves nothing lasting before. The problems are when people underrate it, stay too long to seek testing, stop antibiotics beforehand, or miss advising signs telling them a complication is developing. This infection prices early action and punishes staying every single time. Get tested at first dubitation, start treatment presto, finish the full course, watch for advising signs that escalate the situation, and replace the toothbrush. That is authentically the utmost of what you need to know to handle it well.
FAQ’s
1. How is tonsillitis strep throat different from regular strep?
Tonsillitis strep throat targets the tonsils directly, causing severe lump, pus patches, and violent pain. It carries advanced abscess threat, frequently taking longer recovery despite analogous antibiotic treatment protocols.
2. How long does tonsillitis strep throat last on antibiotics?
utmost cases ameliorate within 24 – 48 hours of starting antibiotics. Symptoms generally resolve in five to seven days, but completing the full ten- day course prevents relapse and ensures full recovery.
3. Can tonsillitis strep throat go down without antibiotics?
It may resolve in healthy grown-ups over seven to fourteen days, but pitfalls of rheumatic fever, abscesses, and order complications make antibiotics the safer, recommended option.
4. Is tonsillitis strep throat contagious and for how long?
largely contagious through respiratory driblets, cases remain contagious until 24 hours after starting antibiotics and fever resolves. Without treatment, contagiousness may last two to three weeks.
5. When should intermittent cases lead to tonsillectomy?
intermittent tonsillitis strep throat generally five or further infections per time for two times — clearances ENT evaluation. Tonsillectomy reduces infection frequency and improves long- term quality of life.
Summary
This condition is common, painful, and fully manageable when handled rightly from the first sign of symptoms. Tonsillitis strep throat treated beforehand with a full antibiotic course resolves fairly in the vast maturity of cases without lasting consequences. The complications rheumatic fever, abscess, order inflammation are nearly entirely preventable with timely, complete treatment. Recreating cases despite proper treatment each time leaves honest ENT discussion about whether surgical junking makes sense. Handle tonsillitis strep throat right the first time, every time, and it stays the manageable infection it was always meant to be.