I got a recurring strep throat for the third time in eight months and authentically started wondering if the commodity was unnaturally broken inside my body. Third positive rapid-fire test, third round of amoxicillin, third week of swab water gargling and sleeping fourteen hours a day. That nine- nanosecond appointment transferred me nearly my croaker presumably did not intend.
Recurring strep throat is not arbitrary bad luck. Certain natural and environmental factors produce advanced vulnerability in specific people and relating which factors apply to your situation is the first step toward breaking the cycle rather than just managing the coming occasion when it inescapably arrives again.
Stay tuned with us as we explore recurring strep throat, its causes, symptoms, treatments, forestallment tips, and expert advice together.
What Recurring Strep Throat Actually Means Medically:

Recurring strep throat has a specific clinical definition that matters practically because it determines what treatment options become available and when. Five or more confirmed strep infections in a single year, or three or more in each of two consecutive years, is the threshold most ENT specialists use when evaluating whether surgical intervention makes sense for a particular patient. Below that threshold the standard approach is treating each episode individually.
What makes recurring strep throat different from just getting unlucky with a common infection is the pattern behind the recurrence. Some patients have genuinely weakened immune responses to Group A Streptococcus specifically. Others have chronically infected tonsil tissue harboring bacteria between acute episodes. Understanding which category you fall into changes what solutions actually make sense for your specific situation rather than the generic average patient population.
Why Some People Get Recurring Strep Throat and Others Never Get It Once:
This was the question I most wanted answered sitting in that pharmacy for the third time. Recurring strep throat is not evenly distributed across the population. Certain biological and environmental factors create meaningfully higher susceptibility in specific individuals and identifying which factors are at play in your own life is genuinely the first step toward breaking the cycle permanently rather than just managing each episode.
Tonsil Anatomy and How It Drives Repeat Infections:
Tonsils with deep crypts and irregular surfaces provide significantly more surface area for bacteria to colonize and more physical hiding spots that antibiotics struggle to fully penetrate even at therapeutic blood levels. After multiple strep infections tonsil tissue undergoes structural changes where normal lymphoid tissue gets progressively replaced by scar tissue serving no immune function whatsoever. Each infection makes the tonsils worse hosts for immune defense and better hosts for bacterial colonization simultaneously.
Immune System Variations Nobody Explains to Patients:
Individual immune systems vary significantly in how they recognize and respond to Group A Streptococcus specifically. Some people mount robust responses clearing bacteria efficiently while others mount responses that are technically adequate but leave enough bacterial load that recolonization happens quickly after antibiotics finish. Neither factor is something patients control directly but both are worth discussing specifically with an ENT specialist during evaluation rather than accepting generic susceptibility explanations without pushing further.
Environmental Exposure Patterns That Overwhelm Indeed Good impunity:
thick work surroundings, classrooms, healthcare settings, and homes with academy- age children produce nonstop strep exposure that overwhelms indeed competent vulnerable systems through sheer frequency and volume of bacterial contact. Recreating strep throat in people working in education or healthcare frequently reflects environmental cargo rather than particular vulnerable weakness. relating exposure patterns helps distinguish between natural vulnerability and situational reinfection taking environmental rather than purely medical results.
The Household Carrier Problem Nobody Talks About:
This was the single most surprising thing I learned during my entire research period and the piece I most wish my doctor had mentioned across any of those three appointments. Recurring strep throat in one household member very frequently traces back to a silent carrier in the same household who is the actual unrecognized source of the cycle. A silent carrier tests positive for Group A Streptococcus on throat culture but experiences absolutely zero symptoms whatsoever.
That person sheds bacteria constantly onto shared surfaces, into shared air, throughout a shared kitchen. The patient with recurring strep throat gets treated, recovers, and gets re infected within weeks from the untested untreated carrier who has genuinely no idea they are the source. This cycle continues indefinitely until the carrier gets identified and treated. Getting everyone in the household cultured regardless of whether they have symptoms is one of the highest-yield interventions available for recurring strep throat and also one of the most consistently overlooked recommendations in standard primary care.
How Incomplete Antibiotic Courses Drive the Pattern:
Most people know the general advice to finish antibiotics. Fewer understand specifically why incomplete courses connect so directly to recurring strep throat rather than just being generally inadvisable. When a ten- day amoxicillin course gets stopped at day five because symptoms are resolved and drug feels inconvenient to continue, the bacteria surviving that partial course are not an arbitrary subset of the original population at all.
What Survives an Incomplete Antibiotic Course:
The bacteria surviving early antibiotic discontinuation are specifically the most antibiotic-tolerant organisms from the original infection. Stopping early selects for these survivors deliberately and leaves them alive in tonsil tissue where they reestablish a subacute infection sitting below the threshold of noticeable symptoms. Recurring strep throat in patients consistently stopping antibiotics early is sometimes actually a single continuous infection that is never fully cleared rather than true independent reinfection each separate time.
Why Feeling Better at Day Four Means Nothing About Bacterial Clearance:
Symptom resolution by day three or four reflects immune response success at controlling the acute inflammatory picture. It does not reflect bacterial elimination from tonsil tissue crypts where bacteria survive in protected pockets with limited antibiotic penetration. Recurring strep throat patients who connect their pattern to incomplete courses often experience dramatically different outcomes simply from completing full courses consistently without making any other changes to their management approach whatsoever.
The Right Way to Complete Treatment and Reduce Recurrence Risk:
Completing the full ten-day course regardless of symptom resolution, replacing the toothbrush at treatment day one, replacing it again at course completion, and maintaining hydration throughout treatment creates the best conditions for genuine bacterial clearance. Recurring strep throat frequency drops meaningfully in patients implementing all three of these simultaneously rather than treating them as optional additions to standard antibiotic therapy already prescribed.
What Your Tonsils Are Doing in Recurring Strep Throat:
The tonsils in patients with recurring strep throat are doing something categorically different from tonsils in people who get strep once and clear it cleanly. After multiple infections tonsil tissue undergoes progressive structural change. Normal lymphoid tissue gets replaced by scar tissue serving no immune function while deep crypts become increasingly ideal bacterial reservoirs where antibiotic penetration is limited and immune access is restricted by the surrounding scarring itself.
This explains why recurring strep throat often becomes harder to treat over time rather than staying consistent in severity and duration. Each episode causes more scarring, more crypt deepening, more structural change making tonsils simultaneously better bacterial hosts and worse immune organs. The tonsils that once protected you become through repeated infection and progressive scarring the primary reason you keep getting sick in the same way repeatedly. Understanding this biological progression explains why tonsillectomy functions as genuine therapy rather than just prevention in high-recurrence patients meeting established clinical thresholds.
The Role of Stress Sleep and Nutrition in Recurring Strep Throat:
Nobody mentioned this connection to me across three separate doctor visits and it deserves significantly more emphasis than it typically receives in standard medical advice. Recurring strep throat does not just reflect bacterial exposure patterns and tonsil anatomy. It reflects immune system capacity and that capacity is directly and measurably impacted by sleep deprivation, chronic stress, and specific nutritional deficiencies in ways documented in research rather than merely intuited from personal observation.
How Habitual Stress Suppresses the Immune Pathways That Fight Strep:
Cortisol released during habitual stress suppresses natural killer cell exertion and specific aspects of the adaptive vulnerable response applicable to bacterial concurrence. Cases developing recreating strep throat during high- stress ages are passing real physiological vulnerable concessions rather than coincidental timing. This does not mean stress causes strep infection directly. It means stress removes the immune buffer that normally prevents each bacterial exposure from becoming a full symptomatic episode requiring antibiotic treatment every single time.
Sleep Deprivation and Its Direct Impact on Strep Susceptibility:
Research consistently shows measurable reduction in immune cell function in people sleeping under six hours per night compared to those sleeping seven to eight hours regularly. During sleep the immune system performs regulatory functions and produces cytokines relevant to bacterial defense that cannot be replicated during waking hours regardless of other health behaviors practiced consistently. Recurring strep throat patients with consistently poor sleep are fighting bacterial infections with a physiologically compromised immune system that adequate sleep would meaningfully strengthen over time.
Nutritional Deficiencies Most Strep Patients Have Never Been Tested For:
Vitamin D insufficiency impairs multiple vulnerable pathways and is extremely common particularly during downtime months when recreating strep throat peaks in frequency. Zinc is needed for normal development and function of neutrophils and natural killer cells contributing to early bacterial concurrence. Iron insufficiency anemia impairs vulnerable function through several distinct mechanisms. Cases with recreating strep throat who have no way had introductory nutritive bloodwork done are missing potentially adjustable contributors to their vulnerability that are straightforward to identify and address virtually.
When Recurring Strep Throat Means Tonsillectomy Is the Right Answer:
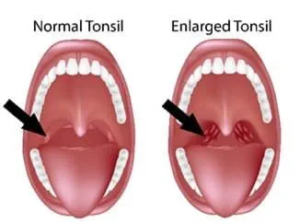
This conversation eventually happened for me after my fifth infection and I want to describe it honestly because the decision is more nuanced than either remove them immediately or never touch tonsils in adults. Tonsillectomy for recurring strep throat in adults is evidence-supported when clinical thresholds are met. It eliminates the chronically scarred bacteria-harboring tissue that has become the primary infection site in high-recurrence patients rather than functioning as the immune defense tonsils were originally designed to provide.
Recovery from adult tonsillectomy is harder and longer than most surgeons communicate upfront honestly. Ten to fourteen days of genuine recovery rather than the five days often suggested casually during pre-surgical consultations. Pain management requires real attention and planning throughout that recovery window. Post-operative bleeding risk is small but real and worth understanding before deciding. For patients meeting recurrence thresholds whose quality of life is being meaningfully impacted by recurring strep throat the recovery investment typically pays back within the first post-surgery year through infections completely avoided.
Recurring Strep Throat in Children Versus Adults:
The experience differs meaningfully between children and adults in ways affecting both decision-making urgency and intervention thresholds significantly. Children have higher baseline strep exposure through school environments, more immature immune systems, and higher complication risk from untreated strep including rheumatic fever disproportionately affecting the five to fifteen age group. These factors push toward more aggressive evaluation and lower thresholds for ENT referral in pediatric recurring strep throat compared to otherwise healthy adults without complicating factors.
Adults face a different risk calculation but not a less important one. Quality of life impact is often higher because adult responsibilities cannot pause for repeated week-long illnesses the way childhood schedules sometimes accommodate. Adults with recurring strep throat are also frequently the household source spreading strep to children who face higher complication risk, which adds urgency to the treatment decision beyond considering only the adult patient’s individual health situation in complete isolation from surrounding family dynamics and household transmission patterns.
Five effects Making Recurring Strep Throat Worse Than It Needs to Be:
The utmost people concentrate only on treating each occasion as it arrives. These habits are laboriously making the pattern worse between occurrences.
- Stopping antibiotics at day five because symptoms resolved directly creates the antibiotic-tolerant bacterial survivors driving the coming occasion of recreating strep throat.
- participating drinks or implements with ménage members during treatment reintroduces bacteria before the throat finishes mending from the current active infection.
- Skipping throat societies during mild illness means missing strep occurrences that still beget tonsil towel damage and contribute to progressive scarring indeed without severe symptoms.
- Keeping the same toothbrush throughout treatment reintroduces streptococcal bacteria twice daily to a throat actively trying to recover from that exact same bacteria.
- Returning to high-stress workloads within days of finishing antibiotics suppresses the immune recovery determining whether the next bacterial exposure becomes another full infection.
Five Warning Signs Recurring Strep Throat Has Become Genuinely Dangerous:
These signs mean the situation has moved past inconvenient territory requiring evaluation beyond another standard antibiotic prescription from primary care alone.
- Throat pain becoming dramatically worse on one side after starting antibiotics suggests peritonsillar abscess forming rather than the infection resolving in expected normal ways.
- Jaw stiffness appearing alongside throat pain during any recreating strep throat occasion is an exigency signal taking same- day medical evaluation without any detention.
- Common pain or casket pain developing during or shortly after a strep occasion suggests rheumatic fever and requires immediate medical attention rather than continued home monitoring.
- Fever returning after compactly perfecting on antibiotics suggests the current antibiotic is not adequately clearing the specific bacterial strain causing this particular recreating occasion.
- Strep confirmed more than five times within twelve months means the clinical threshold for ENT surgical consultation has genuinely been reached and referral is fully warranted.
What Happens to the Body During Years of Recurring Strep Throat:

The long-term picture of inadequately addressed recurring strep throat is not just repeated unpleasant weeks of illness cycling through the same miserable pattern. Chronic tonsil scarring progresses with each infection and does not reverse between episodes during periods of apparent health and normal functioning.
Repeated immune activation against the same bacterial pathogen can in some individuals contribute to the autoimmune complications associated with strep including cardiac valve changes and kidney inflammation developing slowly rather than acutely. Cumulative bacterial load across repeated infections, cumulative antibiotic exposure, and cumulative tissue damage all represent real long-term health costs extending well beyond the immediate suffering of each individual episode experienced in isolation from the larger pattern.
How to Talk to Your Doctor About Recurring Strep Throat More Effectively:
Most primary care appointments addressing recurring strep throat last under ten minutes and result in another antibiotic prescription without addressing the underlying pattern driving recurrence consistently. Changing this outcome requires patients arriving prepared to advocate specifically for a different kind of conversation than the standard reactive prescription visit. Bringing a written log of infection dates, symptom onset, antibiotic courses taken, and whether each course was completed gives the physician data shifting the appointment from reactive prescription writing to genuine analytical evaluation.
Specifically requesting household carrier testing, nutritional bloodwork, and ENT referral evaluation by name rather than waiting for these to be offered unprompted changes what actually happens during those nine minutes significantly. Physicians respond to informed specific requests differently than to general expressions of frustration about getting sick repeatedly without explanation. Knowing the clinical thresholds, knowing the language, and arriving with attestation positions the case as an active party in working the pattern rather than an un resistant philanthropist of the same result applied constantly without meaningful progress toward resolution.
Conclusion
Recurring strep throat is not just bad luck and not a commodity to keep treating identically while hoping the pattern changes on its own ultimately. The ménage carrier dynamic, the deficient antibiotic history, the tonsil towel changes, the nutritive factors, and the stress and sleep connections all represent real and adjustable contributors to why the same infection keeps returning. Understanding which factors are applicable to your specific situation and addressing them totally rather than just treating each occasion collectively is authentically the difference between breaking the cycle and staying inside it indefinitely without resolution.
FAQ’s
1. What officially counts as recurring strep throat by medical norms?
Five or further verified infections annually, or three or further in two successive times, meets the standard ENT clinical threshold for recreating strep throat surgical evaluation consideration.
2. Can a ménage member beget my recurring strep throat without feeling sick?
Yes. Silent carriers test positive for strep bacteria on throat culture without any symptoms and constantly beget recreating strep throat through nonstop unknowing ménage transmission.
3. Will tonsillectomy permanently cure recurring strep throat in grown-ups?
Tonsillectomy dramatically reduces recreating strep throat frequency but does not exclude all threats since remaining throat towels can still come infected after surgery.
4. How does stopping antibiotics beforehand connect to recurring strep throat patterns?
Early termination leaves the most antibiotic-tolerant bacteria alive in the tonsil towel creating a force that reestablishes active infection and directly drives the recreating strep throat pattern.
5. Can nutritive scarcities actually contribute to recurring strep throat vulnerability?
Vitamin D, zinc, and iron scarcities measurably vitiate vulnerable function pathways applicable to bacterial concurrence making nutritive optimization a licit consideration for recreating strep throat cases.
Summary
Recurring strep throat breaks the cycle only when you stop treating occurrences collectively and start addressing the real reasons they keep passing. Household carriers, deficient antibiotics, tonsil scarring, poor sleep, nutritive gaps, and habitual stress all feed the pattern. relating which factors apply to your specific situation and fixing them totally is authentically how recreating strep throat eventually stops.