My daughter was eleven days old when I first noticed something was off. Not dramatically off nothing that would make a stranger look twice, just that particular wrongness you pick up on when you’ve been staring at a tiny human face for eleven straight days and something in the expression shifts in a way you can’t quite name. She wasn’t feeding right. She was quieter than her already-pretty-quiet baseline. And she felt warm in a way that made my stomach drop indeed before I reached for the thermometer.
Strep throat and babe can be serious, as their vulnerable systems are veritably fragile. Indeed mild symptoms like perversity, fever, or difficulty feeding shouldn’t be ignored. Early opinion and treatment help complications similar as dehumidification or secondary infections. Parents should cover nearly and consult a pediatrician incontinently to ensure safe, effective care for their baby.
Learn everything about strep throat and newborns and how to protect your precious baby from this serious bacterial infection today.
Why Strep Throat and Newborns Is a Different Medical Situation Entirely:

The first thing to understand and this is the piece that reframes everything else is that strep throat and newborns don’t behave the way strep throat behaves in literally any other age group. When an aged child or grown-up gets strep, the vulnerable system recognizes the bacterial trouble, mounts a response, and produces the symptoms we associate with the infection — sore throat, fever, blown glands. That response, uncomfortable as it is, is actually the vulnerable system doing its job. Newborns don’t have that same immune infrastructure in place yet. Their immune systems are immature in very specific ways that make bacterial infections not just more dangerous but fundamentally different in how they present and progress.
A newborn with a serious bacterial infection including strep may show almost none of the classic signs that older patients show. No obvious throat pain because they can’t communicate it. Conceivably no fever, or a fever that is subtle enough to miss without a thermometer. Feeding changes, unusual quietness, or just that hard- to- define maternal sense that commodity is wrong are occasionally the only signals available. Strep throat and newborns is genuinely difficult to recognize because the signs are subtle, non-specific, and easy to attribute to the general unpredictability of newborn behavior if you don’t know what you’re looking for specifically.
The Two Types of Strep That Affect Newborns Differently:
Here’s something that confused me initially and I think trips up a lot of parents “strep” isn’t one thing when it comes to newborns. The strep throat that aged kiddies and grown-ups get is Group A Streptococcus, which is what most people mean when they say strep. But when agitating strep throat and babe, Group B Streptococcus is actually the more frequent and more incontinently concerning bacterial trouble, and understanding the difference matters virtually.
Group B Strep GBS is carried vaginally by roughly 25 percent of women without causing any symptoms or health issues for the carrier herself. During vaginal delivery, bacteria can be transmitted to the invigorated, where an immature vulnerable system may struggle to contain the infection.
This is why GBS webbing at 35 to 37 weeks of gestation is standard practice, and why GBS-positive masters admit IV antibiotics during labor to reduce transmission threat dramatically. Strep throat and babe in the GBS environment can develop within the first week of life, occasionally within the first 24 hours, and can progress to sepsis, meningitis, or pneumonia with a speed that makes rapid-fire recognition authentically critical. Group A Strep the throat strep is less common in newborns but does occur, typically through transmission from a household member with active infection rather than during delivery. Both forms deserve serious attention and both require medical evaluation without delay.
How Strep Throat and Newborns Actually Looks in Real Life:
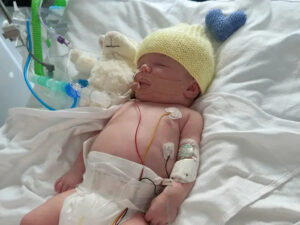
This is the section I wish had existed when I was sitting in that pediatrician’s waiting room trying to mentally inventory every slightly unusual thing my daughter had done in the past 24 hours. Strep throat and newborns doesn’t look like a throat infection looks in an adult. There’s no complaint of throat pain, no pointing to where it hurts, no ability to open wide and show you what’s happening. What you get rather is a collection of behavioral and physical signs that are collectively easy to explain and inclusively worth taking seriously.
Feeding changes are generally the first thing parents notice when a baby who typically feeds well suddenly loses interest, pulling off constantly, acting frustrated or sleepy at the bone or bottle. This happens because swallowing is painful indeed if the baby can not tell you that, and because bacterial infection drains energy reserves that an infant does not have important to spare. Temperature changes either fever above 100.4 degrees Fahrenheit or, occasionally more concerningly, a body temperature that drops below normal are signs that commodity systemic is passing.
Unusual quietness or, again, a high-pitched cry that sounds different from normal hunger or discomfort cries are both worth noticing. Strep throat and newborns doesn’t give you obvious signs, it gives you subtle ones that require a parent who’s paying close attention and willing to trust their instincts enough to call the doctor.
How Strep Reaches Newborns and Where the Transmission Risk Actually Comes From:
Understanding how strep throat and newborns connect from a transmission viewpoint helps parents take authentically defensive action rather than vague, anxious preventative measures that do not target factual threat. GBS transmission happens primarily during delivery, which is why antenatal webbing and intrapartum antibiotics are so effective at reducing it if you are interposing the transmission pathway at its most critical moment. But Group A Strep the throat strep travels a completely different route into a newborn’s environment. Group A Strep lives in the throats of infected people, in respiratory droplets from coughing and sneezing, and on hands that have touched infected surfaces.
In a household with a newborn, anyone with active strep, a sibling, a parent, a grandparent who came to meet the baby represents a transmission risk that’s easy to underestimate because strep in older people looks so routine and manageable. A toddler sibling with strep throat running a low fever and eating normally is still shedding bacteria constantly, still touching things, still wanting to be near and touch the baby. Strep throat and newborns in this household transmission context is one of the more preventable scenarios but only if adults in the household understand the risk clearly enough to take it seriously in the moment.
How Strep Throat and newborns Gets Diagnosed by Croakers:
Opinion in babies is more complex and more critical than opinion in aged cases, and understanding the process helps parents navigate it without the confusion that can decelerate down seeking applicable care. When an invigorated presents with signs that suggest possible bacterial infection fever, feeding changes, unusual geste pediatricians do not approach it the way they’d approach strep in a academy- age child. There’s no “let’s watch it for a day” with a newborn who has a fever. The evaluation is comprehensive and it starts fast.
A complete sepsis workup is typically initiated for any newborn under 28 days with fever; this includes blood cultures to identify any bacteria in the bloodstream, a lumbar puncture to check cerebrospinal fluid for meningitis, urine culture, and chest X-ray if respiratory involvement is suspected. Throat cultures looking specifically for Group A Strep may also be collected. Strep throat and newborns being properly diagnosed requires this level of thoroughness because bacterial infections in newborns can progress to sepsis and meningitis faster than in any other age group, and waiting for definitive culture results before starting treatment isn’t standard practice antibiotics typically begin before results return, adjusted afterward based on what cultures show.
Treatment for Strep Throat and newborns Explained easily:
Treatment in babies is inpatient and intravenous; this is n’t a send- home- with-oral- antibiotics situation, and understanding that ahead of time helps parents not be blindsided by the position of intervention involved when an infant has verified or suspected strep. IV antibiotics allow therapeutic blood levels to be achieved much faster than oral administration, which matters enormously when you’re dealing with an infection that can progress rapidly in an immune system that doesn’t have the reserves older patients have.
Ampicillin and gentamicin are typically the first-line combination used empirically meaning started before culture results return because together they cover the bacterial spectrum most likely to be responsible for newborn infections including both Group B and Group A Strep. Once culture results confirm the specific bacteria and its antibiotic sensitivities, treatment may be adjusted to a more targeted antibiotic. Duration of IV treatment for strep throat and newborns typically runs ten to fourteen days for uncomplicated cases, longer if meningitis or other complications are present. The hospital stay feels alarming to parents who expected to be home with their baby. It’s the appropriate level of response to an infection that genuinely requires it.
Five Habits That Protect Newborns From Strep Exposure:
Protecting against strep throat and newborns starts before the baby comes home and continues through those early weeks when the immune system is most vulnerable and the stakes of an infection are highest. These aren’t overcautious measures, they’re practical steps with direct protective logic behind each one.
- Anyone with active strep symptoms should not visit or hold the newborn until they have been on antibiotics for at least 24 hours and are confirmed fever-free this feels obvious stated plainly but in practice gets negotiated away constantly because people love newborns and want to meet them and don’t fully register that their “mild” strep is a real transmission risk to a baby with an immature immune system that can’t fight back the way they can.
- Hand washing before holding the baby should be non-negotiable for every visitor without exception not a suggestion, not something offered as an option alongside hand sanitizer, but a clear expectation set by parents who understand that Group A Strep travels on hands as readily as it travels through the air. Making this the household rule from day one removes the awkwardness of requesting it case by case.
- Siblings who attend academy or daycare during cold and strep season represent ongoing exposure threat that deserves active covering a academy- age stock who comes home with a sore throat and low fever during the invigorated period should be tested for strep instantly, kept down from close contact with the baby until cleared, and treated incontinently if positive.
- GBS-positive masters should understand their delivery plan easily including timing of antibiotic administration IV antibiotics for GBS-positive maters need to be administered at least four hours before delivery to give maximum protection to the baby during passage through the birth canal. However, this timing may be missed, and neonatal monitoring should reflect that gap meetly, If delivery progresses faster than anticipated.
- Parents who develop sore throat symptoms in the invigorated period should get tested incontinently rather than staying to see how effects develop a parent with untested, undressed strep who’s feeding, holding, and minding for an invigorated around the timepiece is a sustained transmission threat. Getting tested presto and starting treatment snappily protects both the parent and the baby.
Five Warning Signs That Strep Throat and Newborns Needs Emergency Care:
These are the signs that require calling 911 or going directly to the emergency room rather than waiting for a regular pediatric appointment to open up. Strep throat and newborns progressing to serious complications does not wait for business hours.
- Fever of 100.4 degrees Fahrenheit or advanced in any baby under 28 days old is always an exigency anyhow of what differently is or is not present. An invigorated fever is presumed to indicate serious bacterial infection until proven otherwise, and the evaluation needed to rule that out can not be at home or over the phone.
- A baby who becomes limp, unresponsive to stimulation, or surprisingly delicate to wake languor beyond normal invigorated somnolence, particularly in a baby who has lately been feeding inadequately or running a temperature, suggests bacterial sepsis and requires immediate exigency evaluation without any detention for observation.
- Breathing that becomes labored, rapid-fire, murmuring, or involves visible casket retractions respiratory involvement invigorated with suspected bacterial infection suggests possible pneumonia or early sepsis. invigorated respiratory torture changes gormandize and deteriorates briskly than it does in aged children. This is a 911 situation.
- Skin that develops a mottled, bluish, or gray tone color changes in an invigorated body indicating poor rotation or oxygenation are serious anyhow of other symptoms present. Combined with fever or feeding changes in the environment of possible strep throat and newborns exposure, this requires exigency response incontinently.
- A high-pitched, unusual cry that sounds distinctly different from the baby’s normal hunger or discomfort cry occasionally called a neurological cry, this sound pattern can indicate meningeal vexation and should no way be dismissed or attributed to general finickiness when other concerning signs are present alongside it.
What Happens When Strep Throat and Newborns Goes Unrecognized Too Long:
This section exists not to frighten parents but to make the stakes concrete enough that the urgency of early recognition actually lands. Strep throat and newborns that are caught early and treated appropriately carry good outcomes in the majority of cases. Strep throat and newborns that go unrecognized past the early window because the signs were subtle, because parents waited to see if things would improve, because someone assumed the baby was just going through a fussy phase is a different clinical picture with different outcomes.
Group B Strep sepsis that progresses to meningitis can cause permanent hearing loss, developmental delays, and neurological damage even when it’s eventually treated the damage occurs during the period of active infection before treatment begins or reaches therapeutic levels. Group A Strep complications in newborns, including necrotizing fasciitis in very rare cases, pneumonia, and sepsis, progress with a speed that makes hours matter in ways they simply don’t for older patients.
None of this is meant to make parents feel that any hesitation or missed sign means permanent damage; it’s meant to make clear why the medical community is so uniformly aggressive about evaluating newborn fever rather than monitoring it at home. Strep throat and newborns treated promptly does well. The treatment window is real and it’s worth understanding clearly.
Conclusion
Strep throat and newborns is rare, genuinely most new parents will never face it. But rare doesn’t mean impossible, and the gap between recognizing it early and missing it has consequences significant enough to warrant knowing the signs before you need them. Fever in a newborn is always worth calling about. Feeding changes combined with unusual behavior are worth mentioning. Your instinct that something is off is worth trusting enough to pick up the phone.
The medical system’s aggressive approach to newborn fever exists because of exactly what we’ve covered here and working with that system rather than waiting to see if things resolve is how strep throat and newborns get treated early, treated well, and leaves no lasting mark.
FAQ’s
1. Can strep throat and newborns happen in the first week of life?
Strep throat and newborns can absolutely occur in the first week, particularly Group B Strep transmitted during delivery. Strep throat and newborns in this early window often presents as sepsis rather than classic throat infection symptoms. Any fever or feeding change in a baby under seven days old requires immediate medical evaluation without waiting to see if symptoms develop further.
2. How is strep throat and newborns different from strep in older children?
Strep throat and newborns involves an immature immune system that cannot mount the visible inflammatory response older children produce. Strep throat and newborns may show no obvious throat symptoms whatsoever just fever, feeding changes, and behavioral shifts. The diagnostic process and treatment intensity are also completely different, requiring inpatient IV antibiotics rather than oral medication sent home.
3. Can a breastfeeding mama pass strep throat and newborns protection through milk?
Bone milk does contain motherly antibodies including some protection against strep organisms. Still, strep throat and babe threat is n’t excluded by suckling. It’s reduced kindly. A breastfeeding mama with active strep should continue nursing while on antibiotics, as antibiotic situations in bone milk are generally safe and the defensive factors in milk remain salutary throughout infection.
4. How long does treatment for strep throat and newborns generally last?
Strep throat and babe treatment generally involves ten to fourteen days of IV antibiotics in a sanitarium setting for uncomplicated cases. Strep throat and newborns complicated by meningitis requires longer treatment duration, frequently three weeks or further, with ongoing monitoring for neurological goods. Treatment duration is determined by the specific bacteria linked and how the baby responds to cosign antibiotic remedy.
5. Should siblings be kept down during strep throat and newborn treatment?
During active strep throat and babe infection, limiting stock contact reduces fresh bacterial exposure during a vulnerable period. Strep throat and newborns recovery goes most easily when the baby’s terrain is controlled precisely. Siblings with any strep symptoms should be tested and treated before continuing normal contact, and hand hygiene prospects should be maintained constantly throughout the ménage during this period.
Summary
Strep throat and newborns is the kind of topic most parents hope they never need to know in practice. Strep throat and newborns present subtly feeding changes, temperature shifts, behavioral differences that require attentive parents to catch early. Strep throat and newborns treated promptly carries good outcomes in most cases. What makes the difference is parents who know the signs, trust their instincts, understand that newborn fever is always worth calling about, and don’t wait for symptoms to become unmistakable before seeking evaluation. Strep throat and newborns are rare. Your preparation for it doesn’t need to be.







